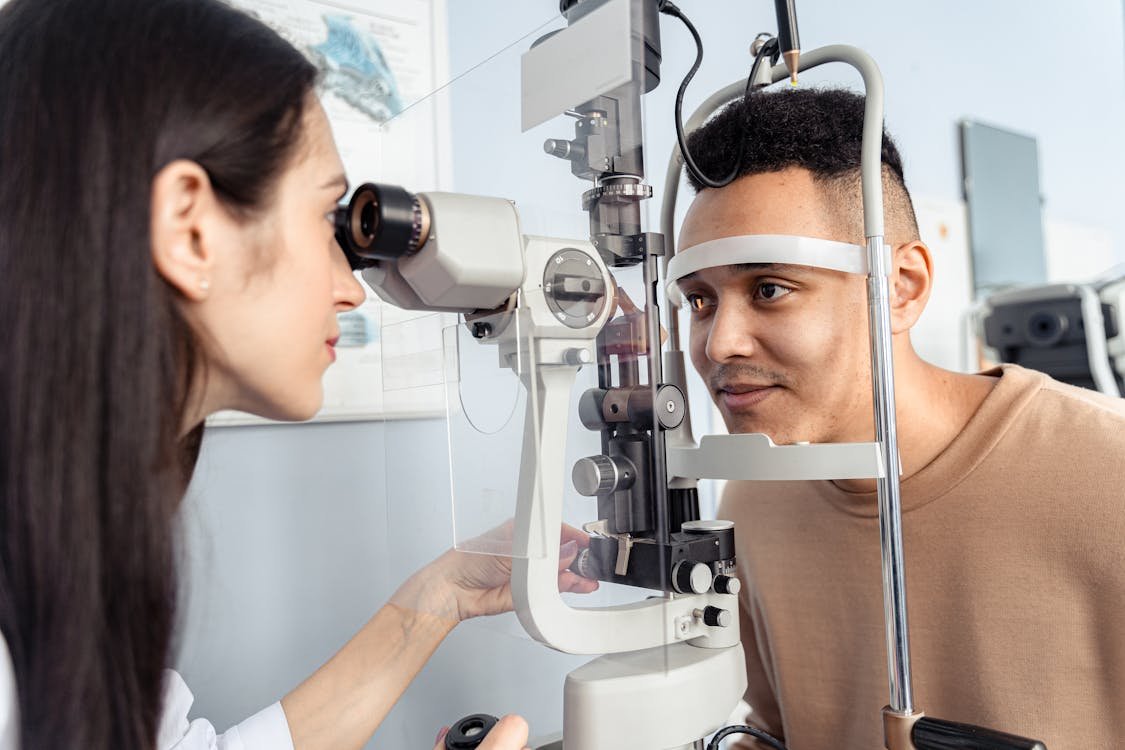
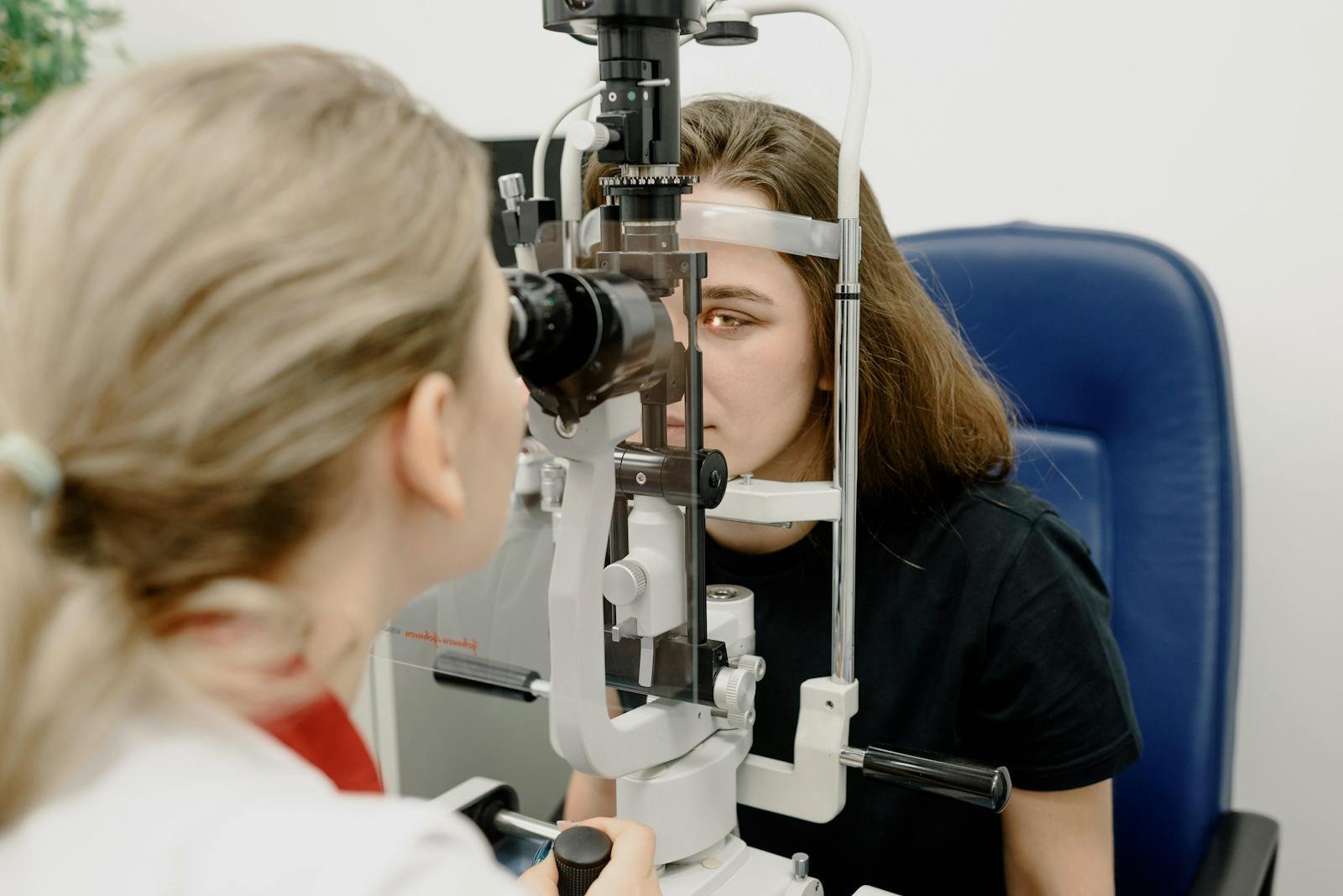
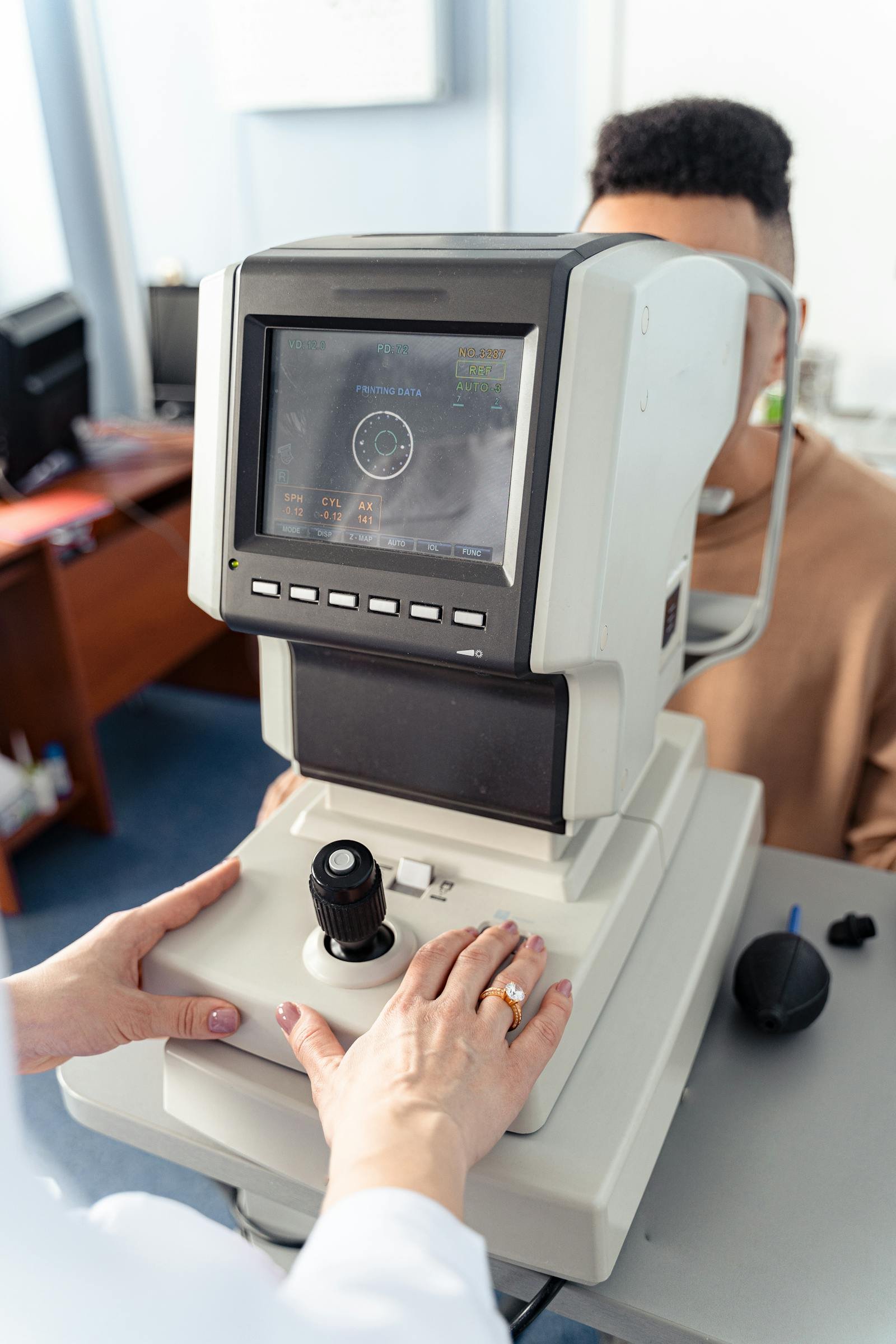
Dry eye disease is one of those conditions that’s been quietly growing for years — and it’s now reaching a point where most opticians see multiple patients a week who are struggling with it. Screen time, ageing populations, contact lens wear, environmental factors — the drivers are everywhere. Yet a surprising number of independent optician practices in the UK still treat dry eye as an afterthought, handing out a leaflet about artificial tears and sending patients on their way.
That’s a missed opportunity on two fronts. First, your patients genuinely need more help than a quick recommendation at the end of a routine eye test. Second, dry eye management represents a real, sustainable revenue stream for your practice — one that doesn’t depend on NHS contracts or frame sales margins.
Setting up a dedicated dry eye clinic within your existing practice isn’t as daunting as it might sound. You don’t need a massive investment or a complete rebrand. What you do need is a structured approach, the right equipment (some of which you probably already have), and a clear patient pathway that turns ad hoc advice into proper, billable clinical care.
Why Dry Eye Matters More Than Ever for UK Opticians
The prevalence of dry eye disease in the UK has been climbing steadily. Research suggests that anywhere between 15% and 33% of adults over 50 experience symptoms, and that figure is climbing in younger demographics too, largely thanks to the amount of time we all spend staring at screens. Post-pandemic working patterns haven’t helped — many of your patients are still spending long hours on laptops in centrally heated home offices, which is basically a recipe for ocular surface problems.
For independent opticians, this presents an interesting dynamic. The NHS GOS sight test doesn’t really accommodate thorough dry eye assessment. You’ve got your 20-odd minutes, you’re checking for pathology, updating prescriptions, and managing referrals. Dry eye gets a mention, maybe, but there’s no time for proper evaluation — and certainly no funding for it.
That’s exactly why a separate dry eye clinic makes sense. It moves the assessment and management out of the standard sight test and into its own dedicated appointment, with its own fee structure. Your patients get better care. You get a clinical service that actually reflects the time and expertise involved.
Getting Started: What You Actually Need
The good news is that you don’t need to spend tens of thousands of pounds to get a dry eye clinic off the ground. Start with what you’ve got and build from there.
Equipment You Probably Already Own
Your slit lamp is the foundation. With good technique and a few additional stains (fluorescein and lissamine green), you can already assess tear film break-up time, corneal and conjunctival staining, and lid margin health. If you’ve got a meibography attachment or an OCT with anterior segment capability, even better — but they’re not essential at the start.
A Schirmer’s test kit costs practically nothing and gives you a quantitative measure of aqueous tear production. Combine that with a validated symptom questionnaire like the OSDI (Ocular Surface Disease Index) or DEQ-5, and you’ve already got a solid baseline assessment protocol.
Worth Investing In Early
If you’re going to take dry eye seriously, there are a few pieces of kit that make a meaningful difference. A meibographer — either standalone or as a slit lamp attachment — lets you image the meibomian glands directly, which is invaluable for diagnosing evaporative dry eye and tracking treatment progress. Patients find the images compelling too, which helps with compliance and understanding.
A tear film analyser like the Keeler TearCheck or similar devices can speed up your assessment and give you objective, repeatable measurements. These typically cost between £3,000 and £8,000, so they’re not trivial purchases, but the return on investment can be solid if you’re seeing enough dry eye patients — and you will be, once word gets out that you offer proper management.
Thermal pulsation devices like LipiFlow or iLux represent the higher end of the investment spectrum (£20,000+), but they’re not necessary to start. You can build a very effective dry eye service without them and add in-practice treatments as your clinic grows and the business case becomes clear.
Building Your Patient Pathway
A dry eye clinic works best when there’s a clear, repeatable pathway for every patient who comes through it. Here’s a framework that works well for independent practices.
Step 1: Identification and Screening
The first step is catching dry eye patients in the first place. Train your team — dispensing opticians, optical assistants, reception staff — to listen for the key phrases: “my eyes feel gritty,” “they water all the time,” “I can’t wear my contacts as long as I used to,” “my vision goes blurry when I’m reading.” These are your triggers.
Add a simple screening questionnaire to your pre-test routine. Even two or three questions about eye comfort, screen time, and environmental factors can flag patients who’d benefit from a dedicated dry eye assessment. When a routine sight test picks up signs of ocular surface disease, that’s your opportunity to recommend a follow-up appointment in the dry eye clinic rather than trying to squeeze everything into the GOS slot.
Step 2: Comprehensive Assessment
Your dry eye appointment should be 30 to 45 minutes. That gives you time to do it properly: detailed history, symptom scoring, tear film assessment (break-up time, Schirmer’s), meibomian gland evaluation (expression, meibography if available), ocular surface staining, and lid assessment. Document everything systematically — this is where good practice management software makes a real difference, letting you record findings in a structured way and track changes over time.
At the end of the assessment, you should be able to classify the patient’s dry eye (aqueous deficient, evaporative, or mixed) and grade its severity. This classification drives your treatment plan.
Step 3: Personalised Treatment Plan
Generic advice doesn’t work for dry eye. Telling every patient to “use drops four times a day” is like telling everyone with a headache to take paracetamol — sometimes it’s enough, often it isn’t, and it doesn’t address the underlying cause.
A proper treatment plan should be layered and specific. For mild evaporative dry eye, that might mean lid hygiene, warm compresses with proper technique instruction, and an appropriate lipid-based lubricant. For moderate to severe cases, you might be looking at in-practice meibomian gland expression, punctal plugs, anti-inflammatory drops, or referral for more intensive treatments.
The key is communication. Explain the diagnosis in plain English, show patients their meibography images if you have them, and set realistic expectations about treatment timelines. Dry eye management is ongoing — it’s not a one-visit fix — and patients need to understand that upfront.
Step 4: Follow-Up and Ongoing Management
Schedule follow-up appointments at appropriate intervals — typically four to six weeks after initial treatment, then every three to six months for stable patients. Each follow-up should repeat the key measurements so you can objectively demonstrate improvement (or identify when a treatment approach isn’t working and needs adjusting).
This is where dry eye management really becomes a sustainable part of your practice. Regular follow-ups build patient loyalty, generate consistent revenue, and position your practice as the go-to for dry eye care in your area. Automated patient recall systems help ensure nobody falls through the cracks — a quick reminder when their next check-up is due keeps the cycle going smoothly.
Pricing Your Dry Eye Service
This is the bit that makes some opticians uncomfortable, but it shouldn’t. You’re providing a specialist clinical service that requires time, expertise, and equipment. It deserves a fair fee.
Most independent practices in the UK charge between £50 and £150 for an initial dry eye assessment, depending on the depth of investigation and the equipment used. Follow-up appointments typically sit in the £40 to £80 range. In-practice treatments like heated meibomian gland expression or IPL can command fees of £80 to £300 per session.
Be transparent about your pricing. Put it on your website, display it in practice, and have your team comfortable explaining what the fee covers and why it’s separate from the NHS sight test. Most patients understand that specialist care costs money — particularly when they’ve been struggling with symptoms that nobody else has taken seriously.
If you’re worried about uptake, consider offering a reduced-rate initial assessment for the first few months to build your patient base and generate word-of-mouth referrals. Once patients experience the difference between a proper dry eye assessment and a two-minute mention at the end of a sight test, they’ll see the value.
Marketing Your Dry Eye Clinic
You don’t need a massive marketing budget to fill a dry eye clinic. Most of your initial patients will come from within your existing patient base — you’re already seeing people with dry eye symptoms every single day.
Start In-Practice
Train your entire team to identify and refer. Put up posters in your waiting area. Mention the clinic on your dispensing receipts and recall letters. Create a simple handout that explains what the dry eye clinic offers and who it’s for. These low-cost, high-impact tactics will generate your first wave of bookings.
Go Digital
Add a dedicated dry eye page to your website with clear information about symptoms, what to expect from an appointment, and how to book. Write blog posts about dry eye management (you’re reading one right now). Share patient-friendly content on your social media channels — tips for managing dry eye at work, the link between screen time and eye comfort, when to see a specialist.
Local SEO matters here. When someone in your area searches “dry eye treatment near me” or “dry eye optician [your town],” you want to be the practice that shows up. Make sure your Google Business Profile mentions dry eye as a service, and encourage satisfied patients to leave reviews mentioning it.
Build Referral Relationships
Connect with local GPs, dermatologists (there’s a strong link between rosacea and meibomian gland dysfunction), and ophthalmologists. Let them know you offer specialist dry eye management so they can refer patients your way. A simple letter or email introducing your service, with a referral pathway attached, can open doors you didn’t expect.
Using Technology to Run Your Dry Eye Clinic Efficiently
Managing a dry eye clinic alongside your regular sight tests and dispensing requires decent systems. You need to be able to schedule dedicated dry eye appointments (longer than standard slots), maintain detailed clinical records that track changes over time, manage recalls for follow-up patients, and handle the private billing separately from GOS claims.
This is where having integrated practice management software really pays off. Rather than juggling separate systems for booking, records, and billing, everything sits in one place. Your clinicians can pull up a patient’s full dry eye history in seconds, compare measurements across visits, and the system handles the recall scheduling automatically.
If your current software can’t accommodate dedicated dry eye appointment types or detailed clinical notes beyond the standard sight test template, it might be time to look at what else is out there. Modern cloud-based systems like Raven Vision are built to flex around the way practices actually work — including specialist clinics that don’t fit neatly into the GOS mould.
Common Pitfalls to Avoid
A few things tend to trip practices up when they’re getting started with dry eye clinics. The biggest one is trying to do too much too soon. You don’t need every piece of equipment on day one. Start with a solid assessment protocol using the basics, prove the concept, and invest in additional technology as the clinic grows.
Another common mistake is inconsistent follow-up. Dry eye management is a long game. If patients attend an initial assessment but don’t come back for follow-up, you’re not providing good care and you’re losing the revenue that makes the clinic sustainable. Systematic recall is non-negotiable.
Finally, don’t underestimate the importance of patient education. Dry eye patients who understand their condition, why treatment takes time, and what they need to do at home are far more likely to stick with the programme and see results. Take the time to explain. Use images. Give them written or digital take-home instructions. It makes a real difference to outcomes and retention.
The Bottom Line
Setting up a dry eye clinic in your independent practice is one of the most practical things you can do to grow your clinical offering and your revenue in 2026. The patient need is there — and it’s growing. The clinical pathway is well-established. The investment required to get started is modest. And the ongoing nature of dry eye management creates the kind of recurring patient relationship that sustains a practice long-term.
You’re already seeing these patients. You’re already qualified to help them. All that’s missing is the structure to do it properly — and charge appropriately for the expertise you’re providing.
Ready to streamline your practice management so you can focus on building specialist services like dry eye clinics? Book a free demo of Raven Vision and see how our all-in-one system handles appointments, clinical records, recalls, and billing — all for £149/month with no lock-in.